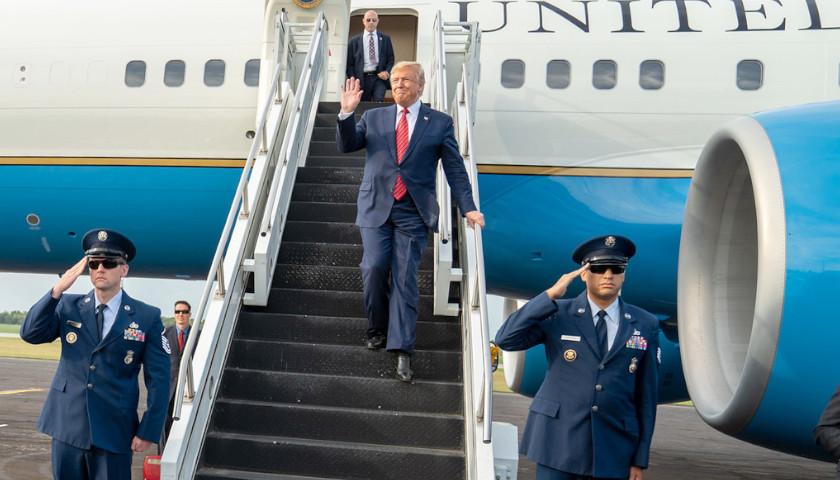by Bethany Blankley
Nineteen attorneys general, led by Indiana, have filed an amicus brief with the U.S. Supreme Court in support of a lawsuit filed by Texas and Missouri against the Biden administration.
They’re asking the Supreme Court to uphold a lower court’s order instructing the Biden administration to follow the law to fully reinstate the Migrant Protection Protocols (MPP), otherwise known as the “Remain in Mexico” policy.
“No one is above the law in America, and we are simply insisting that the Biden administration follow the law,” Indiana Attorney General Todd Rokita said (pictured above).
“The rule of law is the framework that enables American liberty to survive and thrive,” he added. “The situation at our southern border provides the perfect example of how going soft on the rule of law gives rise to anarchy, chaos, and ultimately the erosion of our freedom and safety.”
In January 2021, President Joe Biden announced via executive order that he was terminating MPP. Months later, Department of Homeland Security Secretary Alejandro Mayorkas began dismantling it and other immigration policies. Southern border encounters then surged to historic levels. In Biden’s first year in office, Customs and Border Protection and Border Patrol agents encountered or apprehended roughly 2 million people entering the southern border illegally. This number excludes the several hundred thousand who are estimated to have evaded law enforcement.
At the same time, Mayorkas implemented a wide range of policy changes to effectively halt most deportations. CBP and Border Patrol agents were directed to release illegal immigrants into the U.S. en masse instead of sending them back to Mexico to go through the immigration process.
Texas and Missouri sued, District Judge Matthew Kacsmaryk of the Northern District of Texas granted their request for a permanent injunction and ordered the administration to reinstate the MPP. He ruled the administration violated the Administrative Procedure Act when it halted the MPP.
The administration appealed to the Fifth Circuit and U.S. Supreme Court and lost. Both courts denied its request to stay Kacsmaryk’s ruling.
After its Supreme Court loss, the administration said it was appealing Kacsmaryk’s ruling, vowing to “vigorously challenge it.” In a statement, it said, “As the appeal process continues, however, DHS will comply with the order in good faith. Alongside interagency partners, DHS has begun to engage with the Government of Mexico in diplomatic discussions surrounding the Migrant Protection Protocols.”
But compliance hasn’t happened, as evidenced by the flood of illegal immigrants the administration is releasing into the U.S. and by the tactics it’s used in court to circumvent the law, the AGs argue.
“From the beginning of this Administration, the United States has been forthright about its intention to terminate MPP simply because it did not like the program, and its conduct demonstrates its readiness to do anything – including ignore the APA’s requirements – to accomplish that objective,” they argue in the brief.
“The Administration’s ‘act now, justify later’ approach began on Inauguration Day, when it summarily paused MPP,” they add.
Throughout the appeals process, “the Fifth Circuit correctly concluded that the United States’ efforts to avoid judicial review violated basic principles of procedure,” they argue.
An unprecedented number of people are expected to come through the southern border after the administration ends the Title 42 public health authority May 23, the attorneys general have argued, necessitating the urgency for the Supreme Court to weigh in.
Implemented under President Donald Trump in January 2019, the MPP led to a reduction in the number of people entering the U.S. illegally. The Trump administration also invoked Title 42 to enable CBP and Border Patrol agents to quickly expel illegal immigrants and prevent entry to a greater number of people during a public health emergency.
Current law requires those not authorized to enter the U.S. to be detained, to stay in Mexico, or be “paroled” into the U.S. based on narrowly defined case-by-case circumstances including “urgent humanitarian reasons or significant public benefit.”
The Biden administration has been issuing paroles en masse to release illegal immigrants into the U.S., the attorneys general argue, violating the law.
The administration maintains it’s inherited a flawed system, and its policies are more humane than the previous administration’s. White House press secretary Jen Psaki told reporters last December after the administration lost another court battle in the case, “it is not our preference to be reimplementing and reinstituting the Migrant Protection program. … we still feel that the program is inefficient, inhumane, and we are not – we weren’t, we were – did not eagerly reimplement it.”
– – –
Bethany Blankley is a regular contributor to The Center Square.
Photo “AG Todd Rokita” by AG Todd Rokita.