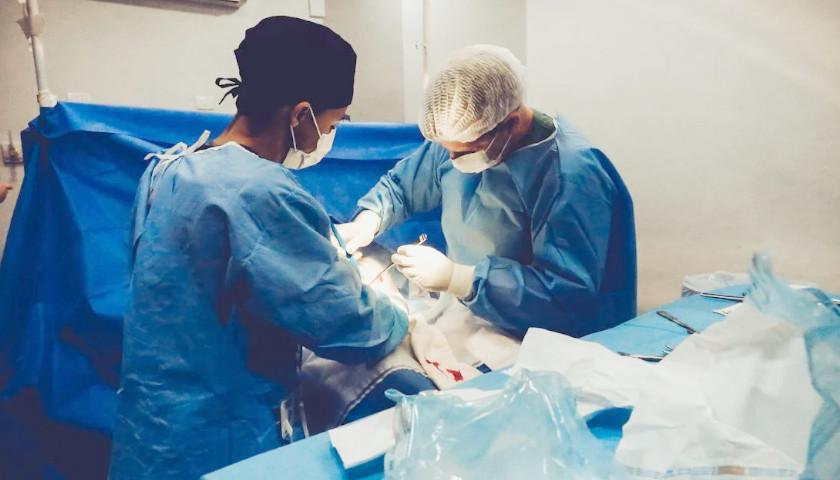
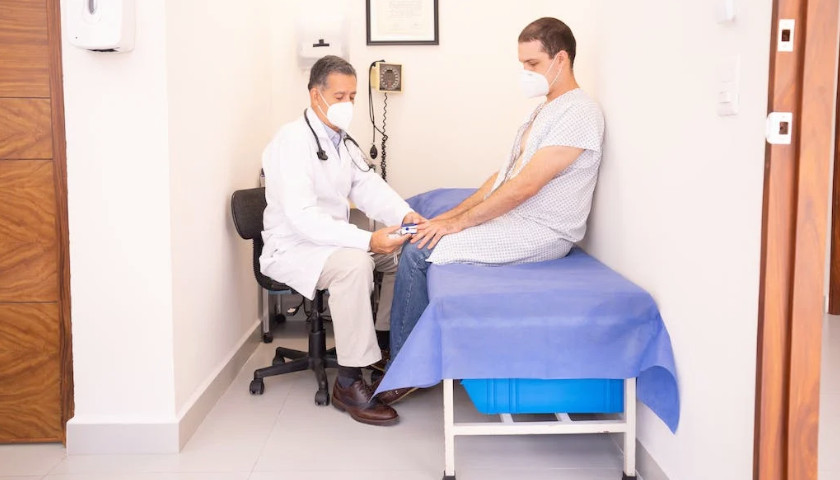
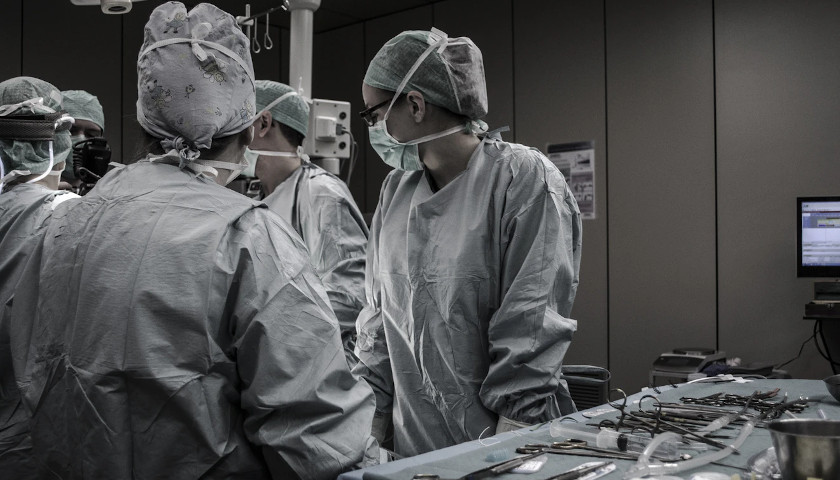
The Virginia Hospital & Healthcare Association (VHHA) announced the rebranding of its VHHA Shared Services division, which delivers products and resources to help Virginia hospitals and health systems improve their clinical, financial, and operational performance.
Read the full storyTag: hospitals
Virginia Hospital and Healthcare Association Launches Campaign Focused on Educating the Public About Health Care Law Reforms
The Virginia Hospital & Healthcare Association (VHHA) announced Monday the launch of a new public awareness campaign focused on making sure patients and families in Virginia “know their rights to help them make informed medical decisions.”
Read the full storyStudy: Many Hospitals Profited During COVID Pandemic
A new study reveals that nearly 75 percent of all U.S. hospitals were able to post positive operating income at the height of the Chinese Coronavirus pandemic, primarily due to relief funds provided by the government.
As Axios reports, the analysis by JAMA Health Forum shows that the average hospital’s operating margins – the difference between revenue and expenses – hit an all-time high in 2020 and 2021, the first two years of the pandemic. Many hospitals continue to post improving operating margins even after 2022 despite the rising inflation, which some have attributed to the massive profits in the first two years of COVID.
Read the full storyPennsylvania Republicans Consider Paths to Hospital Price Transparency
A committee of GOP Pennsylvania lawmakers on Thursday gathered in downtown Lewisburg to consider ways to make patients aware of hospital service prices ahead of time.
At the House Republican Policy Committee hearing at the Open Discourse Coalition headquarters, policy experts testified that, despite a new federal rule requiring price transparency, many hospitals still fail to accurately inform patients of procedures’ costs. Representative David Rowe (R-Middleburg), who organized the event, recalled constituents telling him they’ve faced shocking examples of pricing opacity.
Read the full storyLamont’s Health Care Cost-Cutting Plans Face Pushback
Connecticut Gov. Ned Lamont’s plan to control health care costs in the state is facing blowback over claims it would cost hospitals hundreds of millions of dollars in lost revenue.
Lamont’s proposal, which is being considered by the Legislature’s Joint Committee on Public Health, calls for reducing costs that often get tacked on to consumers’ medical bills, such as facility fees that charge patients for the use of medical and hospital offices during treatments, which he says would save the state’s consumers $400 million a year.
Read the full storyDozens of Hospitals Have Closed in States That Expanded Medicaid, Research Shows
Medicaid expansion has failed to prevent hospital closure, with almost 50 shutting down in expansion states since 2014, according to research given exclusively to the Daily Caller News Foundation.
The research from the Foundation for Government Accountability (FGA) indicates that while Medicaid expansion was intended to solve hospitals’ finances and job shortage, its “empty promises” have done the opposite, report author Hayden Dublois wrote. Hospitals instead have had to shut their doors, lost thousands of jobs and racked up substantial losses, amounting to a loss of almost 5,400 beds.
Read the full story‘Fuel Poverty’ Stresses Pennsylvania’s Hospitals
Pennsylvania’s hospital administrators say rising energy costs driving worldwide “fuel poverty” threaten the stability of the entire U.S. health care system.
“Folks can’t pay to heat their homes,” Chuck DiBello, vice president of facilities and real estate for the Allegheny Health Network, told the Senate Majority Policy Committee. “They get sick and they come to the hospital – sometimes just to get warm.”
Read the full storyBeacon Center of Tennessee Releases Healthcare Access Report Highlighting the Barriers Posed by Certificate-of-Need Laws
The Beacon Center of Tennessee released a report Thursday highlighting challenges to healthcare access in the state posed by Certificate-of-Needs (CON) laws.
Read the full storyOhio Hospitals Using Robot Pharmacy Dispensers to Minimize Errors
Hospital Pharmacies around the state have begun implementing robots to distribute inpatient medication orders to minimize human error.
The XR2 Automated Central Pharmacy System, manufactured by Omnicell was first introduced in 2017. The 30-foot-long robot is capable of dispensing thousands of inpatient medication orders daily.
Read the full storyReport: 78 Percent of Georgia Hospitals Are Not Following Federal Accurate Pricing Law
A year-and-a-half after a law requiring hospitals to post accurate prices online went into effect, roughly three-quarters of Georgia hospitals continue to hide the cost of care from consumers.
That’s according to a new report from PatientRightsAdvocate.org. The organization reviewed 2,000 of the 6,000 accredited hospitals nationwide and found that a mere 16% complied with a federal hospital price transparency rule that took effect on Jan. 1, 2021.
In Georgia, 78% of hospitals are non-compliant.
Read the full storyGov. Kemp Plans to Use $217 Million in Federal Funds for Georgia Healthcare Facility Grants
Georgia Gov. Brian Kemp plans to use more than $217 million in federal money to fund grants for hospitals, assisted living communities and personal care homes.
The state will use money from the American Rescue Plan’s (ARP) Coronavirus State and Local Fiscal Recovery Funds for grants to bolster COVID-19 response efforts.
Read the full storyCommentary: Joe Biden’s Failed Policies Has Lead to a COVID Test Shortage
America has basically run out of tests for Covid-19 as lines are forming at emergency rooms, urgent care facilities and doctors’ offices, and now patients are simply being turned away nationwide. In the meantime, tests are being rationed to those with greater risk factors just a month after President Joe Biden was pushing “test to stay” in order for Americans to be allowed to go to work, school and to travel.
This comes as the Institutes for Health Metrics and Evaluation (IHME) project an estimated 1.9 million probable Covid infections in the U.S per day — and rising. By the end of January, IHME estimates as many as 2.8 million new cases per day, largely thanks to the new omicron variant that accounts for 95 percent of all new cases, the Centers for Disease Control say.
For perspective, last year, IHME estimated cases peaked at over 500,000 a day in early Jan. 2021.
Read the full storyHospitals Are Getting Away with Ignoring Price Transparency Rules, Experts Say
Many hospitals are not complying with laws requiring them to make their healthcare prices publicly available, according to multiple reports, and the Biden administration has so far refrained from issuing penalties.
The Hospital Price Transparency rule, which went into effect Jan. 1, 2021, is designed to promote competition in healthcare markets by requiring hospitals to post their prices, so that consumers can compare and shop between hospitals. The law mandates hospitals to post their pricing data “as a comprehensive machine-readable file with all items and services” as well as “in a display of shoppable services in a consumer-friendly format.”
However, according to recent reports, many hospitals have yet to comply with the rules a year after they have been in effect. An investigation by The Wall Street Journal last week found that many of the nation’s largest hospital chains were not complying with the new rules.
Read the full storyOhio National Guard Called to Help with Hospital Staffing Shortages
More than 1,000 Ohio National Guard members began working in hospitals across the state Monday to help combat what Gov. Mike DeWine called a growing strain caused by the rising number of COVID-19 hospitalizations.
The Ohio Department of Health also has begun working with a staffing company to bring more nurses and other providers from out of state to help ease pressure on current hospital staffs as the number of patients hospitalized with COVID-19 has reached its highest level of the year.
“While the staff will be concentrated in the places where they are most needed, the entire state will feel relief as the arrangement supports the coordination of patient care that has been happening really since the beginning of this pandemic,” DeWine said at a news conference.
Read the full storyFacing Labor Shortages, Several Large Hospital Systems Drop Vaccine Mandates
Several large U.S. hospital systems have dropped their COVID-19 vaccine requirements for employees in the wake of a U.S. district court’s temporary halt of the Biden regime’s vaccine mandate for healthcare workers.
After months of protests, the mandate forced thousands of hospital employees to either resign, or be terminated because of their refusal to get vaccinated.
Louisiana-based federal Judge Terry Doughty issued a preliminary injunction on November 30, blocking the federal government from mandating the experimental injections for workers at Medicare or Medicaid-funded healthcare facilities in 40 states.
Read the full storyNurses in Illinois Win Temporary Restraining Order Against Vaccine Mandate
An Illinois judge granted a temporary restraining order to nurses who sued Riverside Healthcare over the hospital system’s vaccine mandate.
Kankakee County Judge Nancy Nicholson granted a temporary restraining order until Nov. 19. She will then hold a hearing on a motion for a preliminary injunction requested by the nurses.
Read the full storyFlooding Could Wipe Out 25 Percent of Critical Infrastructure: Report
About 25% of critical infrastructure in the U.S., or 36,000 facilities, is at serious risk of being rendered inoperable as a result of flooding over the next three decades, according to an industry report released Monday.
American infrastructure such as police stations, airports, hospitals, wastewater treatment facilities, churches and schools were all considered in the analysis, according to First Street Foundation, the group that published the first-of-its-kind report. The U.S. is “ill-prepared” for a scenario where major flooding events become more commonplace, the report concluded.
Read the full storyCOVID Case Numbers Surge in New England, Despite Region Having Highest Vaccinate Rate in U.S.
Hospitals across New England are reporting full intensive care units and staff shortages as a result of COVID- related illnesses that are starting to impact care, despite the region having the highest vaccination rates in the country.
Public officials say the record case counts, hospitalizations and deaths that rival pre-vaccine peaks are largely among the unvaccinated and are pleading with the part of the population to get the shots, according to the Associated Press.
Read the full storyHealth and Human Services Whistleblower Calls Federal Government’s COVID Policies ‘Evil at the Highest Level’
A medical professional who works for the Department of Health and Human Services (HHS) is blowing the whistle on the federal government for pushing dangerous experimental vaccines on an unsuspecting public, calling the malfeasance “evil at the highest level.”
“You have the FDA, you have the CDC, that are both supposed to be protecting us, Registered Nurse Jodi O’Malley told Project Veritas founder and CEO James O’Keefe, “and everything that we’ve done so far is unscientific.”
The whistleblower works at Phoenix Indian Medical Center, an Arizona hospital run by the Indian Health branch of HHS, but perhaps not for long. After contacting O’Keefe, she recorded some of her HHS colleagues raising concerns about the COVID vaccines. Putting her faith in God, O’Malley said that after everything she had witnessed, she was willing to lose her job to expose the federal government’s counterproductive and destructive COVID policies.
Read the full storyNew Federal Rule: No More Surprise Hospital Bills and More Options for Consumers
Hospitals have begun publishing their actual costs of services, including discounted cash and negotiated rates as a result of a rule change implemented by former President Donald Trump. The rule was challenged by the American Hospital Association and others, who lost in federal district court.
An appeal to the court ruling has not yet been filed. While the association says it is calling on the new administration to adjust the rule, hospitals in the meantime must publish prices for the majority of the services and medications they provide.
Read the full storyCommentary: Five Ways Hospitals Can Help Fix Vaccine Rollout Debacle
Hospitals have come under sharp criticism for their part in the chaotic COVID-19 vaccine rollout. That’s because in the rush to get the vaccine out quickly, many hospitals were shipped more vaccine than anticipated and fewer staff took it than anticipated. As a result, hospitals accrued a vaccine surplus and offered it to their low-risk grad students and young administrative staff working from home and are now scrambling to figure out what to do with the rest. The answer should be simple: give it to older members of your community, but a recent letter from the American Hospital Association cited a number of important barriers to effective vaccine distribution including a lack of coordination and guidance from federal, state, and local governments.
Read the full storyUS Breaks Single-Day Record of New Coronavirus Cases
The United States recorded nearly 37,000 new cases of the novel coronavirus Wednesday as the virus continued to spread across southern and western states, according COVID-19 trackers.
The 36,880 new cases is up from 34,700 recorded Tuesday, and broke previous single-day record for new cases set April 24 when 36,739 were confirmed, according to a New York Times database.
Read the full storyOhio Issues an Order to Delay Elective Surgeries to Preserve Personal Protective Equipment
The Ohio Health Department announced an order Tuesday that told hospitals in the state to postpone non-life threatening surgeries and procedures in order to safeguard personal protective equipment (PPE) for health care workers.
Read the full storyOpentheBooks Oversight Finds the Top 82 U.S. ‘Non-Profit’ CEOs Rake In Nearly $300 Million, Net Assets Reach $200 Billion
by Adam Andrzejewski The rising cost of healthcare is undermining the American Dream. Families who are working hard to get ahead now pay nearly $20,000 per year in insurance premiums, deductibles, and out-of-pocket costs for healthcare. Our OpenTheBooks Oversight Report – Top 82 U.S. Non-Profit Hospitals, Quantifying Government Payments & Financial Assets – studied the largest charitable healthcare providers. Last year, patients spent roughly one out of every seven U.S. healthcare dollars within these healthcare networks. These powerful institutions are organized as public charities – not as for-profit corporations. Any profits must be re-invested into their charitable mission, yet last year, their combined net assets increased from $164.2 billion to $203.1 billion – that’s 23.6 percent growth.* Meanwhile, their executives are highly compensated. Collectively, $297.5 million in cash compensation flowed to the top paid executive at each of the 82 hospitals. Here’s how executive compensation breaks down at the 82 largest non-profit hospitals using the IRS 990 informational returns and auditing the latest year available: 13 organizations paid their top earner between $5 million and $21.6 million; 61 organizations paid their top executive between $1 million and $5 million; Only eight organizations paid their top earner less than $1 million (which…
Read the full storyHospitals’ Secret Contracts With Insurers Are Keeping Health Care Expensive: Report
by Evie Fordham Hospital systems are making secret contracts with insurers that are keeping health care costs high, a Wall Street Journal report revealed, prompting alternative health care advocates to point out the flawed nature of the U.S. health care system. “Health care is the only industry I can think of where technology is used as an excuse for price to go up and productivity to go down because of these perverse incentives,” The Health Rosetta founder Dave Chase told The Daily Caller News Foundation. “The perverse incentives at a high level are generally, either directly or indirectly, the worse job [the hospitals] do, the more they get paid.” TheWSJ’s Tuesday report detailed “dozens of contracts with terms that limit how insurers design plans” so they cannot exclude powerful hospital systems, which when included in health plans can drive up costs for employers and employees. These secret contracts often include clauses that mandate insurers steer consumers away from less costly health care providers or give hospitals the ability to “mask” their prices, according to TheWSJ. If plans did not include these more costly health care systems, they could be up to 10 percent cheaper, the report stated. Some major health…
Read the full story